Ask most people whether green spaces are good for health and you’ll get a fairly confident “yes”. The evidence backs them up. Time spent in parks, woods, gardens, coasts and waterways is linked to lower stress, better mental health, more physical activity, and greater social connection. For people experiencing health problems and even other disadvantages, that connection with nature may be especially powerful. Green spaces potentially act as a health equaliser in communities where access to other health-supporting resources is limited.
So, here’s the question those of us who evangelise about the health benefits of green spaces don’t ask nearly often enough: who isn’t going?
Around a quarter of the UK population visits green or blue spaces less than once a month. In Scotland, NatureScot surveys put that figure at roughly 26%. Research across 33 European cities found comparable numbers. These aren’t people who lack green spaces nearby. Many of them live within walking distance of a park. Yet for a complex web of reasons, some visible, some much harder to see, they simply don’t go.
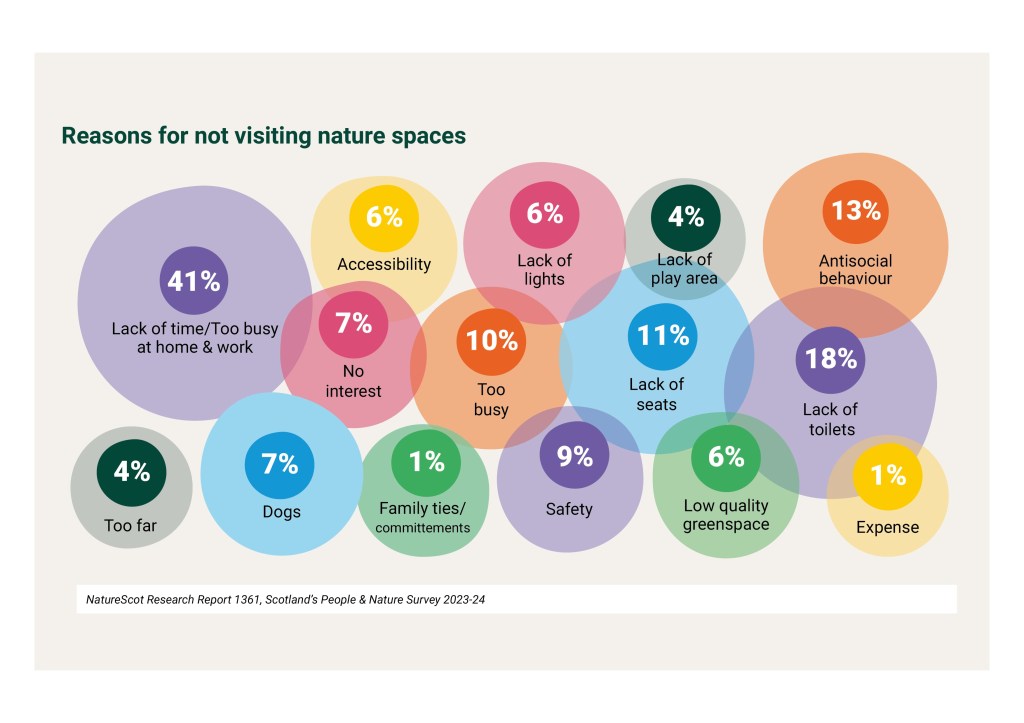
This is what we call the ‘green gap’ and it matters enormously, because the people least likely to visit green spaces are disproportionately the same people who stand to benefit most from them: those with long-term health conditions, people from lower socioeconomic backgrounds, older adults, people with disabilities, and people from minority ethnic groups. In other words, the very populations for whom a regular walk in the park could make the biggest difference are the ones researchers, policy makers and practitioners have consistently failed to reach.
Until now, research and policy have had no coherent framework for thinking about why.
Introducing the Green Gap Framework
Published in Landscape and Urban Planning, the Green Gap Framework is the first theoretical framework designed specifically to map and explain non and low use of urban greenspaces. Developed by members of CRESH, Rob Bushby, and the GroundsWell consortium, the framework is the product of an extensive iterative process involving literature review, expert consultation, and collaboration with over 100 researchers, policymakers, planners, practitioners, and members of the public across the UK, Europe, and beyond.
What the framework offers is something deceptively simple but genuinely novel: a shared language and a structured way of thinking about all the reasons someone might not visit a green space. Not just the obvious ones. The framework organises these reasons across four interconnected domains.
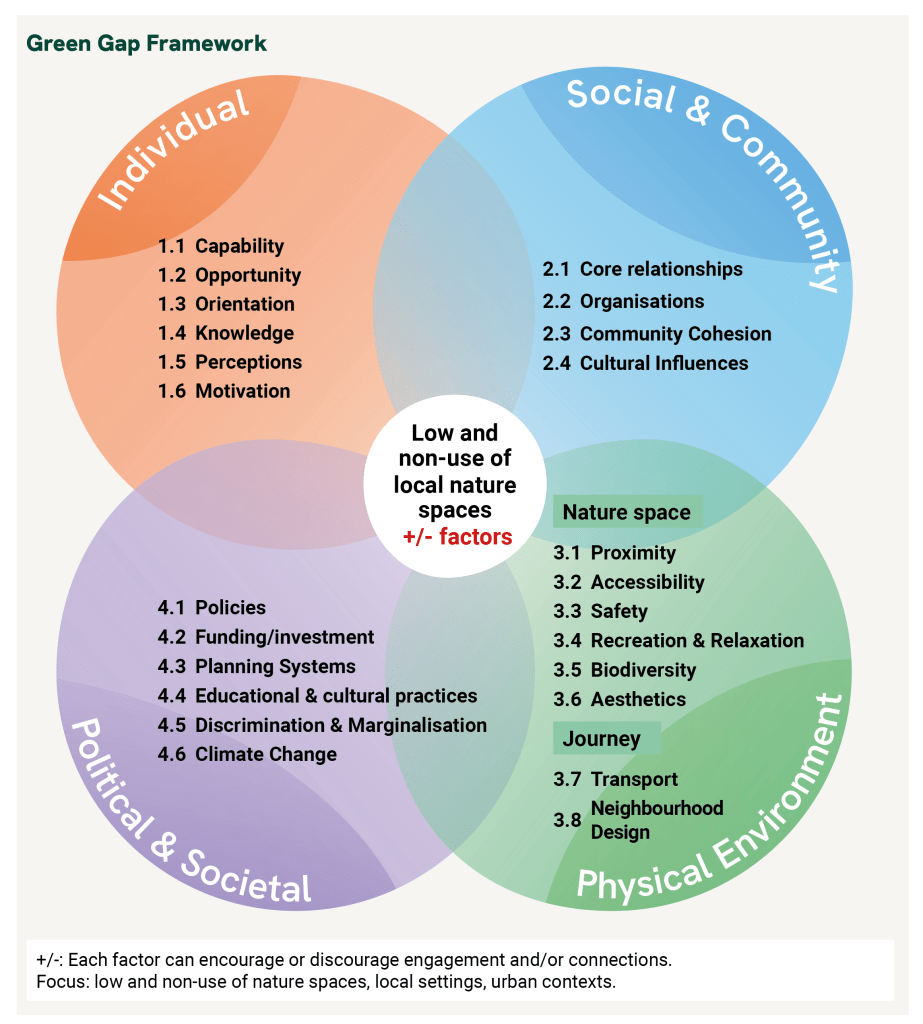
Domain 1 – Individual. This covers the factors unique to a person: their physical and mental capability to visit, the time and opportunity they have, their knowledge of what’s nearby, their attitudes and prior experiences, and – crucially – their motivation or lack of it.
Domain 2 – Social and Community. Whether or not someone visits a green space is also shaped by the people and groups around them; family members and friends who model or discourage outdoor habits, community organisations, schools and employers, the cohesion and perceived safety of a neighbourhood, and the cultural significance (or absence) of green spaces in someone’s background.
Domain 3 – Physical Environment. This is where most existing policy and research has focused; the characteristics of green spaces themselves (proximity, accessibility, safety, aesthetics, biodiversity, facilities for recreation) as well as the journey to get there (transport links, neighbourhood design, roads and infrastructure). These factors matter enormously, but they’re not the whole story.
Domain 4 – Political and Societal. Perhaps the most overlooked domain: the policies, funding decisions, planning systems and cultural practices that shape which communities have well-maintained, welcoming green spaces and which do not. This domain also considers discrimination and marginalisation, and the impacts of climate change.
Each factor in the framework is marked with a +/− symbol to reflect an important insight: the same factor that enables one person to use a green space may be the very thing that prevents another. Dogs in a park are a draw for some visitors and a deterrent for others. A park that feels safely secluded to one person may feel isolated and threatening to another.
What Makes This Different?
Previous greenspace research has tended to ask, ‘what are the benefits of green spaces, and how do we design better ones?’ Those are valuable questions, but they assume the barrier is primarily a physical one; if you build it well enough, people will come.
The Green Gap Framework challenges that assumption directly because interventions that focus only on physical improvements risk missing the deeper drivers of non-use and, at worst, can actively worsen inequalities.
The framework also makes a deliberate and important methodological choice. Earlier drafts organised barriers around demographic categories: age, sex, ethnicity, disability. These were replaced with attitudinal and trait-based factors. The reason is significant: the framework’s purpose is not to predict in advance which groups won’t visit green spaces, but to explain why any group or individual might not, and to identify where intervention could help. This shift makes it far more useful across different communities and contexts.
A Tool Built for Use and Change
The framework was explicitly designed to be used beyond academia. We worked throughout its development with planners, park managers, third-sector organisations, and members of the public to ensure it would be genuinely applicable in the real world.
The framework is designed to evolve. We have been very clear that this is not a finished product. Like the influential frameworks by Markevych et al. and Lachowycz and Jones that have shaped greenspace and health research, the Green Gap Framework is intended as a living tool, refined as empirical evidence accumulates and as different communities engage with it.
The Bigger Picture
Health inequalities are widening. The populations most affected by poor health are also those with the least access to the things that protect and restore health, including green space. At a time when public health budgets are under severe pressure, the case for low-cost, scalable interventions that can reach the people who need them most is urgent.
Green and blue spaces are, in principle, free to access. They exist in or near most urban communities. They have a robust and growing evidence base for physical and mental health benefits. The problem is not the spaces themselves. The problem is the complex, multilevel web of barriers, individual, social, environmental, and systemic, which prevent too many people from using them.
The Green Gap Framework doesn’t solve that problem, but it gives us, for the first time, a coherent way to think about it and a shared foundation from which researchers, planners, policymakers and practitioners can begin to work on it together.
Find out more
We have more information and assets for you, including a plain-language summary guide for practitioners and policy makers.
The Green Gap Framework paper is published open access in Landscape and Urban Planning: https://doi.org/10.1016/j.landurbplan.2026.105663
More resources, insights and use cases are available on the Green Gap section of the Groundswell website.
GroundsWell is funded by the UK Prevention Research Partnership (MR/V049704/1).