We recently developed a project summary for an ESRC-funded study looking at the impact of the financial crisis and subsequent austerity measures on mental health and wellbeing in the UK. The summary for the CRESH project (full title: Recession, austerity and health: changing area socio-economic conditions and their relationship to individual health and wellbeing outcomes in Scotland) includes the key findings, links to papers published, details of some of the dissemination activities, and other useful resources. You can read more in the pdf below:
Category: wellbeing
-
What next for tobacco control in Scotland?
New research from the CRESH team using data from 124,566 shopping baskets purchased in convenience stores across Scotland has found that the purchase price of tobacco is lower in more disadvantaged neighbourhoods, largely because of the higher sales of the cheapest brands in these areas.
Cigarette smoking is one of the leading causes of preventable ill-health, hospitalisations and deaths in Scotland. Approximately 19% of adults in Scotland smoke, this rises to 32% in our most deprived fifth of neighbourhoods and falls to 9% in the most affluent neighbourhoods. As Scotland moves towards a ‘Tobacco Endgame’ the Scottish Government have a target to reduce smoking prevalence to less than 5% by 2034. A recent review of smoking projections by CRUK however suggests that Scotland may miss this target by 16 years in the poorest neighbourhoods. It is important that we continue to explore all potential determinants of smoking, particularly those that drive smoking in our most deprived communities.
We know that tobacco price is one of the most important determinants of smoking behaviour and that many smokers are price sensitive. Whilst it may appear that all tobacco products are becoming increasingly expensive, research suggests that the average tobacco price in the UK has remained relatively unchanged in real terms over the past 20 years in spite of numerous tax increases. A practice, known as ‘undershifting’, has seen tobacco companies limit price increases on the cheapest brands and instead increase the price of the most expensive brands by larger margins, thus absorbing the tax increases on the cheapest cigarettes allowing them to remain cheap (Hiscock et al. 2018). As a result, the price of the lowest priced cigarette brands has remained relatively steady and the tobacco market as a whole has become increasingly stratified by price between the cheapest ‘sub value’ , ’value’, ‘mid price’ and high priced ‘premium’ brands. We wanted to understand these differentials in price a little better, so we carried out some research that was published recently in Tobacco Control. We explored whether the price paid for tobacco (both cigarettes and roll your own tobacco) was different in different types of neighbourhoods. We compared areas by deprivation, by the density of tobacco outlets and by rurality.
We analysed tobacco purchase data provided to us by The Retail Data Partnership. We looked at more than 124,000 purchases in 274 stores across Scotland in April 2018. For cigarettes the average price paid for a pack of 20 was £8.49, ranging from £7.20 to £13.25. For roll your own tobacco (RYO) 30g the average price paid was £12.14, with prices ranging from £9.80 to £15.99. We found that the price paid for tobacco did vary by neighbourhood type. In neighbourhoods with the lowest average household income the average purchase was 50p less for a pack of 20 cigarettes, and 34p less for roll your own tobacco compared with the most affluent neighbourhoods.
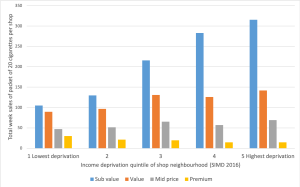
We then asked whether this was driven by individual brands being cheaper in more deprived areas, or whether cheaper, sub-value, brands were just more popular in such places. We found little evidence that individual brands were priced differently. Although the cheaper brands are the most popular in all neighbourhoods and across Scotland, accounting for 52% of sales, there’s a big difference in popularity between more and less deprived areas, In the most deprived areas these brands account for 58% of sales, but in most affluent areas it was just 39% (See Figure 1 below). So, it is the dominance of cheaper brands in more deprived areas that drives the 50p difference in average price paid per pack between deprived and affluent areas. Remember this matters because the tobacco companies work to subdue tax-based price rises on the cheapest brands.
We also explored whether the density of tobacco retailers and/or rurality had an impact on tobacco price. We found little evidence of a density effect, but we did find that the individual brands analysed were significantly cheaper in rural areas.
So what does this mean and what can we take from this research? It is clear from the CRUK review that we need to work harder in order to reach the 2034 target of less than 5% of the population smoking. Price is a lever that we can pull, but to date this has been largely done through tax increases. This research shows us that the cheapest brands are the most popular in all neighbourhood types, but much more so in our most deprived neighbourhoods where smoking rates are highest. We found that the price paid for tobacco is lower in more deprived areas compared to more affluent areas. Our results confirm that the dominance of cheaper, so called ‘sub-value’ brands in more deprived areas, is a driving force behind the difference in price paid for tobacco between neighbourhoods. This highlights the importance of cheaper tobacco products to the consumer and the market. Cheap tobacco may help tobacco companies to retain price sensitive consumers who live in the most deprived areas, which, in turn, contributes to health inequalities. In addition to increases to the duty rates on tobacco, more radical policy responses are likely to be required. These include a combination of minimum unit pricing (MUP) and a price cap at the upper end. The MUP would raise the cost of cheaper cigarettes and the price cap at the upper end would prevent the more expensive brands being used to ‘protect’ the cheaper ones from tax rises.
With growing international interest in the ‘Tobacco Endgame’, policymakers should identify measures that counter industry tactics that enable the continued sales of cheap tobacco. We published this paper in the first week of the COVID-19 pandemic in the UK. These are clearly strange times and we should rightly focus on the public health impacts of the global pandemic, and in particular the vast health inequalities that are arising. We must not however forget that the public health challenges we were faced with before this pandemic remain. Tobacco, and other unhealthy commodities, require our attention and the inequalities that arise from them remain a matter of social justice.
You can find the paper here:
References
Hiscock R, Branston JR, McNeill A, et al. Tobacco industry strategies undermine government tax policy: evidence from commercial data. Tob Control 2018;27:488 LP – 497. doi:10.1136/tobaccocontrol-2017-053891
-
New ESRC funded study on Tobacco and Alcohol
We are delighted to announce that we have been awarded funding from the ESRC for a project exploring tobacco and alcohol environments in Scotland. The project ‘Change in alcohol and tobacco availability, population health and the lived experience’ will be funded for 3 years, beginning December 2019 for a total of £761, 470. The project will be led by Professor Niamh Shortt with co-investigators from the University of Edinburgh (Professor Jamie Pearceand Dr Tom Clemens), Glasgow Caledonian University (Professor Carol Emslie) and the MRC/CSO Social and Public Health Sciences Unit, University of Glasgow (Professor Richard Mitchell).
This research will measure change in the availability of alcohol and tobacco in Scottish neighbourhoods over time and explore how this change relates to health outcomes and how residents experience the availability of alcohol and tobacco in their neighbourhoods. The findings will be important because smoking and alcohol consumption are leading causes of illness and death. In Scotland smoking causes one in every 5 deaths and one in 20 deaths is related to alcohol. This harm is not equally shared; those on the lowest incomes suffer the greatest harm. These illnesses and deaths are preventable. The World Health Organisation recommends that nations prioritise interventions that reduce the supply of alcohol and tobacco.
Why might neighbourhood supply of alcohol and tobacco matter? Research suggests that when there are a lot of outlets in a neighbourhood this impacts upon consumption in three ways. 1. The outlets may be more competitive and drive prices down to attract customers. 2. Oversupply may normalise the products when they are sold alongside everyday commodities, such as bread and milk. 3. Tobacco and alcohol may simply be easier to buy in areas where there are more outlets.
In order to explore the relationship between supply, behaviour and harm we need data on the location of every outlet in Scotland selling tobacco and/or alcohol. Ideally, to be able to say something about whether the relationship may be causal, we need this data over time. We have already collected data on the specific location of every outlet selling tobacco and licensed to sell alcohol over multiple time periods (2012 and 2016 (nationwide alcohol and tobacco – see paper here) and 2008 (alcohol in four cities – see paper here)). As part of this project we will collect updated data for 2019/20. This will allow us to measure this change over time. Using an approach called trajectory modelling we will group neighbourhoods that have had a similar degree of change; some neighbourhoods may have lost, or gained, local shops or pubs, whereas some may not have changed at all. We will then identify features of these neighbourhoods that may be driving this change, for example the age profile of the population or poverty levels. This will help policy makers understand the drivers of change in our neighbourhoods.
To measure the relationship between changing supply and harm we will link these trajectories, and our measures of availability at each time point, to alcohol and tobacco health outcomes (behaviour, illness and death). We will use statistical models to see whether areas experiencing an increase or decrease in outlets have seen a corresponding increase or decrease in these outcomes. This will allow us to get a better understanding of whether an over supply of alcohol and tobacco is related to smoking and alcohol consumption and harm. These findings will provide important evidence related to the provision of such commodities in our neighbourhoods.
Although these statistics are important to report we also need to understand why an oversupply of alcohol and tobacco may influence behaviour and harm. Whilst the literature suggests the pathways listed above, we know little about the experiences of individuals living in neighbourhoods with contrasting availability. We don’t understand the individual experience of any of these pathways. Professor Carol Emslie will lead a qualitative work package and researchrs will meet with groups of individuals, in neighbourhoods of contrasting trajectories, to talk to them about the supply of alcohol and tobacco. We will explore their experiences of neighbourhood and assess how their perceived notions of their neighbourhood availability contrast with our statistical measures. Finally, we will meet with residents, retailers and policy stake-holders to explore potential interventions related to supply. Policies at this level require public, retailer and political support. We will discuss the priorities held by various groups, present our quantitative results and gauge attitudes towards potential interventions.
Throughout the project will be committed to knowledge exchange, public events and speaking with non academic partners. If you wish to know more about this research, or would like one of the researchers to come to your organisation to provide you initial findings (once the project is under way) then contact the Principal Investigator here: niamh.shortt@ed.ac.uk
-

Mental health problems are common among prisoners in low-income and middle-income countries
In a major international review, we found very high rates of psychiatric and substance use disorders among prisoners in low-income and middle-income countries. The results from the systematic review and meta-analysis published in Lancet Global Health showed that the prevalence of psychosis, depression, and drug and alcohol use disorders is much higher in this marginalised population in comparison to the community, pointing to unmet needs and calling for action in research and policy.
Mental health and substance use problems are common among individuals involved in the criminal justice system. Incarcerated men and women often come from disadvantaged socioeconomic and family background, and frequently have a life history of victimisation and substance use, making them more vulnerable to mental health problems. While in prison, they often remain undiagnosed and untreated. Prisoners with unmet mental health needs have higher mortality, especially by suicide, and greater risk of recidivism and reoffending after release in the community, leading to multiple imprisonments.
Although 70% of the worldwide prison population are residing in low-income and middle-income countries (LMIC), almost all scientific evidence is coming from studies conducted in high-income countries. It is an important limitation as recommendations from a mostly Western context might not be applicable or generalizable to poorly resourced settings. Prison conditions in LMICs are usually very harsh, characterised by overcrowding, poor nutrition, and sanitation, and limited or complete lack of access to basic health care. To provide evidence for future research and policy making, we conducted a systematic review and meta-analysis on prison prevalence studies in LMICs.
After screening 6000 titles and abstracts from 17 electronic global databases, we identified 23 relevant publications based on 14,527 prisoners from 13 different LMICs. Considering a one year time interval, approximately 6.2% of the prisoners had psychosis, 16.0% major depression, 3.8% alcohol use disorders, and 5.1% drug use disorders. To illustrate the immense burden of mental health problems, we quantified the difference between the prevalence among prisoners in each sample and in the sex-matched general populations of the respective countries. Prevalence rates among prisoners were 16 times higher for psychosis, 6 times higher for major depression and illicit drug use disorder prevalence, and twice as high for alcohol use disorders, indicating a significant public health concern and large unmet health care needs in this marginalised group. Moreover, rates in prison populations of LMICs might be even higher than in high-income countries.
Based on our findings, we presented several implications and recommendations for research and policy.
- While a review from 2012 on prison mental health in high-income countries identified over 100 samples, we were able to find only 23 studies from a much larger and diverse group of countries. There is a need further evidence from LMICs to adequately plan interventions for prisoners with mental disorders, especially from regions underrepresented in research such as Central and East Asia, and Central America.
- Because correctional facilities in LMICs often lack basic health care, the implementation of cost-effective interventions and scalable treatments for individuals with mental health problems is crucial.
- Imprisonment could present an opportunity to treat people with mental health and substance use problems who otherwise would be difficult to reach for health services. National governments in LMICs should move the responsibility for prison health care from prison administrations to the national health services.
- Since human right violations, and physical and psychological abuse are more common in resource-poor correctional settings, increasing mental health literacy among staff and protecting the rights and health of people with mental illnesses should be a priority for penal justice policies.
The invited comment on our paper gives a valuable and very practical recommendation on how to improve mental health services in correctional facilities. Training prison health workers by mental health professionals using the WHO’s Intervention Guide for mental disorders (mhGAP-IG), could be a cost-effective and valuable programme for addressing the treatment gap among prisoners in LMICs and coming closer to the Sustainable Development Goals declared by the United Nations.
By Gergo Baranyi, PhD Student in Human Geography and Marie Sklodowska-Curie Early Stage Researcher, The University of Edinburgh
-
What is ‘on the ground’ in a city linked to levels of inequality in life satisfaction
In a European-wide study of 63,554 people from 66 cities in 28 countries, we found links between urban design and levels of inequality in life satisfaction. This is the first study to theorise and examine how the entire urban landscape may affect levels of and inequalities in wellbeing in a large international sample.
Cities with an even distribution of facilities, housing and green space were linked with lower levels of inequality between residents’ life satisfaction levels, suggesting that more equal access to a range of facilities and types of land may help reduce the gap in life satisfaction between the most economically-deprived and most affluent residents of a city.
There was a strong link between higher life satisfaction and living in cities with homes surrounded by natural, green space. However, lower life satisfaction was linked to living in cities that had more wasteland, more space dedicated to housing, and more space in which all the land is concrete or tarmacked.
Implications for policy and planning.
The findings of our study suggest that urban planning has a role to play in addressing inequalities in cities. Our finding that more equal distribution of land cover/use is associated with lower levels of socio-economic inequality in life satisfaction supports the idea that city environments could be equigenic – that is, could create equality.
What people want or need from their city varies moment to moment, day to day, life stage to life stage. If a city is varied enough to offer people what they need, when they need it, it is likely to support a higher quality of life.

Why understanding city design is important for population health and well-being?
With the United Nations reporting that more than half the world’s population residing in urban areas and this proportion rising, it is important to understand how well-planned urban environment might improve, and reduce inequalities in, quality of life. Therefore, understanding the influence urban environments can have on all aspects of health and wellbeing is increasingly important. Cities are continuously evolving and there is ample opportunity to ensure these are healthier and happier place to live.
What we did:
We applied theory and methods from landscape ecology to explore associations between cities’ land cover/use, residents’ reported life satisfaction and within-city socio-economic inequalities in life satisfaction. We joined individual-level responses to the European Urban Audit (EUA) Perception Surveys (2012 and 2015) with city-level data from the European Urban Atlas classifying land cover/use into 26 different classes. Our sample included 63,554 people from 66 cities in 28 countries.
The study, ‘Are urban landscapes associated with reported life satisfaction and inequalities in life satisfaction at the city level? A cross-sectional study of 66 European Cities’ is published in Social Science & Medicine (Open Access). The work was funded by The Medical Research Council (MRC) and Scottish Government Chief Scientist Office.
By Rich Mitchell, Natalie Nicholls & Jon Olsen , Neighbourhoods and Communities programme, MRC/CSO Social and Public Health Sciences Unit, University of Glasgow.
-
Changing places and mental health: do changes in perceptions of neighbourhood influence anxiety and depression in adults?
Written by Dr Jon Olsen, Research Associate with the Neighbourhoods and Communities programme, MRC/CSO Social and Public Health Sciences Unit. This blog is mirrored on the SPHSU website.
Mental health problems are a global issue. In 2013 over 615 million individuals suffered from anxiety and/or depression across the world, a rise of 50% since 1990. How people experience their local environment can impact on mental health. Living in areas that are perceived to have higher levels of neighbourhood problems such as poor housing quality, limited amounts of greenspace, industrial activity, and high traffic volume, has been linked to poorer mental health by some research studies. But, few studies have explored how change in what people think about their neighbourhood is linked to change in their mental health. It would be useful to know this as improving the neighbourhood environment could strengthen mental health.
In our recently published study, we wanted to see how changes in what people thought about their neighbourhood impacted on residents’ mental health over time. We looked at two mental health outcomes: anxiety and depression. Adults who lived in West Central Scotland, an area including Glasgow and eight neighbouring local authorities, were asked to complete the same questionnaire in 1997 and 2010.

Glasgow, United Kingdom – October 20, 2013: People come to walk around and shop at the historic Barras Market Place flea market. What did we find?
Overall, anxiety and depression in the people we spoke to reduced between 1997 and 2010. However, those who experienced worsening neighbourhood perceptions from 1997 to 2010 also had increased anxiety and depression scores.
Why this matters
Our study showed that worsening neighbourhood perceptions were linked with small increases in anxiety and depression scores. People living in areas where perceptions of the neighbourhood got worse, did not benefit from the general improvements in anxiety and depression scores enjoyed by the population as a whole; this could widen health inequalities.

Wheelie bins (blue for recycling, green for general refuse) lined up for collection in a Glasgow alley. The take home message from this study
There is a clear need for national and local policy to target areas where neighbourhood conditions are substantially deteriorating to ensure people’s mental health does not suffer.
Further information about the study
We used data from the Transport, Housing and Well-being study; a postal survey of adults in eight local authority areas in the west of Scotland in 1997 and 2010. More information and a link to the full questionnaire can be found here: http://thaw.sphsu.mrc.ac.uk/.
Anxiety and depression was measured using the Hospital Anxiety and Depression Scale (HADS), a common measure of psychological distress that has been in use for over 30 years.
The full paper was published in the International Journal of Environmental Research and Public Health and is freely available here.
Disclaimer: The views expressed in this blog are those of the author.
The MRC/CSO Social and Public Health Sciences Unit is funded by the Medical Research Council and the Scottish Government Chief Scientist Office. The views expressed are not necessarily those of the Medical Research Council or the Scottish Government.